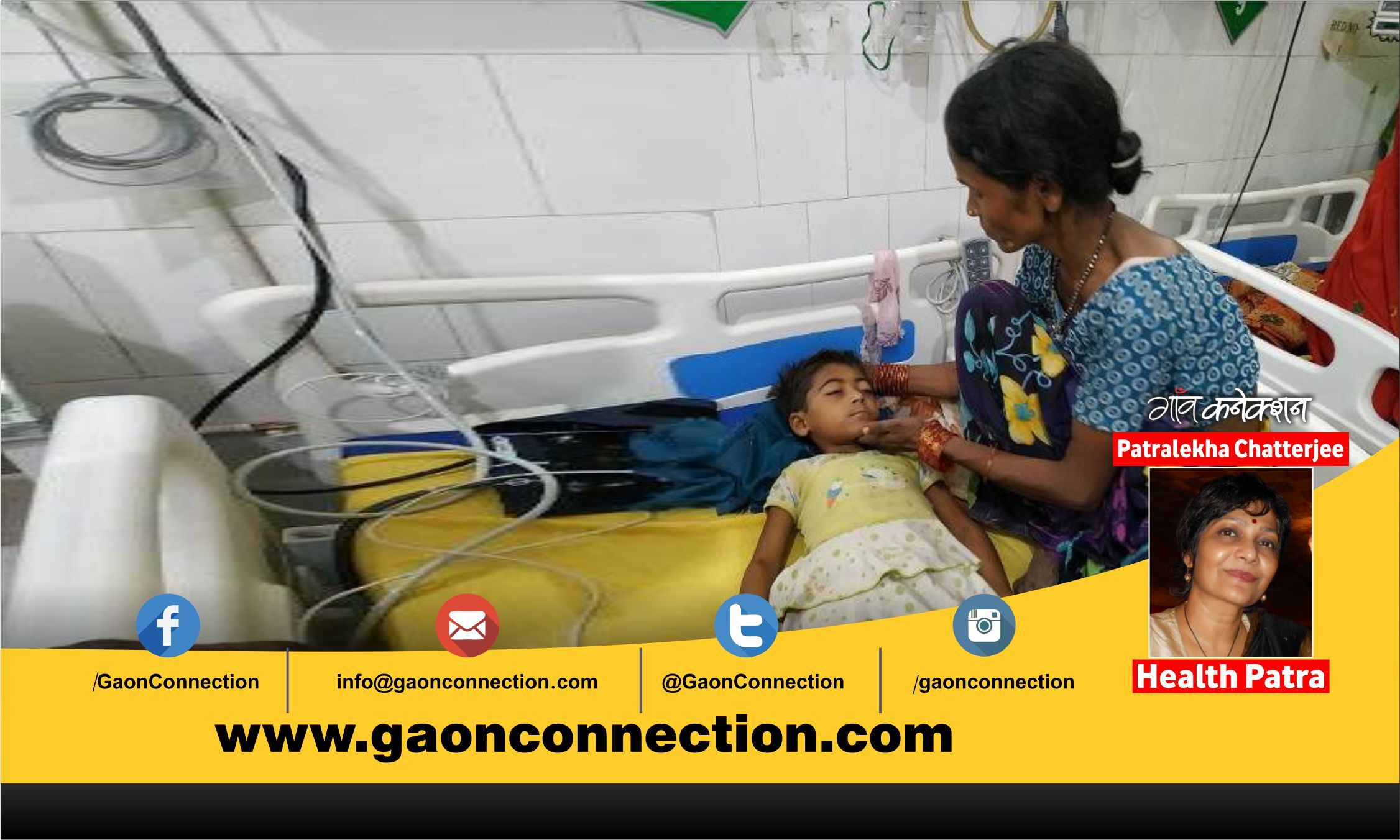
Cut the clutter
There are many theories swirling around about the exact epidemiological causes that has claimed the lives of nearly 150 children in Muzaffarpur, Bihar’s lychee belt, and the adjoining districts since the beginning of June this year.

Patralekha Chatterjee 25 Jun 2019 7:51 AM GMT
Wading through the flood of words about the recent child deaths in Bihar's Muzaffarpur district, one stark fact leaps out. The children could have been saved. It did not need rocket science. Nor much money.
There are many theories swirling around about the exact epidemiological causes that has claimed the lives of nearly 150 children in Muzaffarpur, Bihar's lychee belt, and the adjoining districts since the beginning of June this year.
The most exotic theory in the early days pivoted around lychees or rather the toxin in the lychee. Now we know, the lychee was not the sole culprit.
There were other critical factors at play like child undernutrition and a creaky public health care system which just could not step up the plate.
Meanwhile, lychee farmers have taken a hit due to the mindless initial stigmatisation of the lychee.
The deaths are being pinned on a neurological illness called Acute Encephalitis Syndrome or AES. Most of the deaths have been attributed to low blood sugar level (hypoglycaemia).
The point to remember here is that victims were children of a lesser God. The toxin in the lychee triggers a range of chemical reactions which can be fatal only if the children are undernourished and have gone to bed without a proper meal.
Rich or middle-class children don't die if they eat lychees because their parents usually make sure they have had a meal before they go to bed.
These children had no such luck.
A series of lapses on the part of the State, the community and their families snuffed out their lives prematurely.
They died because they came from poor families in one of India's poorest states; they were chronically undernourished; the anganwadi centres in the area were not in good shape.
In 2016, only around 40% of Bihar's children had received ICDS services. The primary health centres were also woefully short of manpower and resources. Their parents were not sufficiently aware about the risks of letting children go to sleep on an empty stomach.
I called up Dr T Jacob John who was previously a professor of virology at the Christian Medical College in Vellore. John has retired but continues to live in Vellore. He knows the terrain and the issue well.
He told me just two simple measures could have saved the children. First, they would perhaps be alive today if their parents had made sure they had a proper cooked meal before going to sleep. Second, if they had been given 10% dextrose (a form of glucose) intravenously within four hours of the onset of symptoms.
This can be done quite easily in a primary health centre. You don't need even cold chain facilities to store glucose. A medical doctor at the PHC can administer dextrose. If a doctor is not there, a staff nurse can do the job.
John was speaking from experience. He and other doctors, including Dr Arun Shah, a Muzaffarour-based paediatrician, had been invited some years ago to investigate this so-called mystery disease which struck Muzaffarpur and nearby areas with monotonous regularity since 1995. The doctors investigated the outbreaks in 2012, 2013 and 2014. They found that infusion of 10% dextrose within four hours led to complete recovery of the sick children.
That is all that it takes to save lives. Why is something that is actually so simple being made to sound complicated?
A report that was published in the internationally renowned medical journal, The Lancet, in 2017 and which referenced the research done by John and his colleagues noted that 'This recurring outbreak of acute encephalopathy is associated with both hypoglycin A and MCPG toxicity from litchi consumption, 'The study also pointed out that 'this illness is also associated with absence of an evening meal.'
The lament over the lychee has helped obfuscate many critical issues. Like child malnutrition in places like Muzaffarpur and the lapses on the part of the State. These are topics which the political class predictably does not want to talk about.
But the fact is that though India aspires to be a Superpower, we fare miserably in the hunger stakes.
Forty three per cent of Indian children under five years are underweight and 48 per cent (i.e. 61 million children) are stunted due to chronic undernutrition, according to UNICEF. Undernutrition is substantially higher in village India compared to urban areas.
John says their studies showed that all children who were affected by AES were below ten years. They symptoms started manifesting early morning, from 4 am to 6 am, and the incidents occurred mostly between the months of April, May, and June, during the lychee harvesting season. Most of the affected children were from families camping in the orchards for lychee harvesting and had free access to a lot of lychees.
The point to note here is that they were overwhelmingly under-nourished and the toxic reaction had set in because they had gone to sleep on an empty stomach.
John and his colleagues had visited the primary health centres in Muzaffarpur and instructed the doctors and advised that frontline workers about what to do bring to down mortality and morbidity due to AES among children in Muzaffarpur district.
That standard operating procedures had indeed been laid down is evident from letters written by an additional secretary in the Union Health Ministry to health officials in the state health departments in Bihar as well as West Bengal in October 2015.
The letters urge the state governments to involve frontline workers like ASHAs and ANMS to deliver the necessary key messages to the community. The 2015 letter also highlights the need to strengthen diagnostic and critical capacity at all levels of health care to enable timely diagnosis and management of 'acute encephalopathy; cases.
So, there had been attempts to put in place health systems. For some time, it even looked as if things were working. The number of sick children came down quite sharply in 2015 and 2016.
So, what happened this year? Did complacency kick in? Were awareness drives by frontline workers given a toss because of elections?
One can only speculate. But clearly, there has been slippages in 2019.
Dr Arun Shah, the Muzaffarpur-based paediatrician who was part of the research team that included John, says a massive awareness programme is necessary in the communities that are at risk before the onset of summer to' not allow children to go to sleep without meal, not allow them to eat lychees on an empty stomach .Primary health centres also need to be strengthened so that there is trained medical staff round the clock to deal with emergency cases.
That is easier said than done. We come to the other elephant in the room - Bihar is woefully short of doctors,
"The problem of non-availability and uneven distribution of skilled health care providers is the central challenge towards meeting the health goals in Bihar," says the Bihar Economic Survey 2018-2019.
There are 3146 regular doctors in Bihar, against 7249 sanctioned posts, indicating a high vacancy ratio of 57 percent. In addition, there are also sanctioned posts for 2314 contractual doctors, of which only 533 posts have been filled up, representing again a high vacancy ratio of 77 percent," the Survey points out
(Views are personal)




